 While seemingly rare, it is an important clinical consideration given theĬorrect circumstances and should not be overlooked in the emergency department. Prolonged QT is perceived as a clinical specter that is transiently considered on an academicīasis when we approach a patient with syncope or order one of the many medications that canĮlongate the interval. Identification of differences in the pediatric and adult ECG aid in distinguishing potentially life-threatening abnormalities from a normal ECG, with one of the most notable and vastly overlooked conditions being prolonged QT interval. This percentage was shown to be higher when a group of teenagers in intensive physical training were analyzed. Around 10% can develop transient, asymptomatic Mobitz Type I 2nd degree AV block at rest. Additionally, these adolescents can have a prolonged PR interval at rest - some to the extent they have ongoing 1st degree block while sleeping. Bradycardia at rest is often seen in young, healthy and mostly athletic teenagers. Of note, healthy teenagers can have significant abnormalities on ECG that are normal variants. Age-based charts are available and should be referenced when determining appropriate PR interval and QRS complex duration. 2 Both P wave and QRS slowly widen to adult ranges as the child ages. The PR interval initially shortens in the first year of life before gradually widening to the adult range through childhood. It is important to remember that what may be a normal PR interval in an adult can be a manifestation of 1st degree block in a young child.Īdditionally, a normal adult QRS could be a bundle branch block in a young child. This is often overlooked because most of us have committed normal adult wavelength ranges to memory. 1,3Ĭhildren have shortened PR intervals and QRS complexes compared with adults. 
These Q waves are expected, so much so that their absence in the lateral leads can be an indication of congenital heart disease. Other characteristics that would raise concern would be right precordial Q waves, wide Q waves, abnormally deep Q waves. They can be as deep as 8 mm in lead III during childhood. Young children can have a significant Q wave in the inferior and lateral leads from birth until age 3-5 years, when they recede. 
2 The T waves in V5 and V6 should always be positive after the first 3 days of life. Presence of a positive T wave in V1-V3 past the first week of life is pathologic and warrants further investigation. Occasionally, this pattern can last later into adolescence and young adulthood. 1,2,3Ī pediatric norm that can initially seem alarming to an adult practitioner is the “juvenile T-wave pattern.” The precordial leads have T-wave inversions that normally persists until age 10-12 years. Similarly, as the left ventricle grows during the first years of life, a decrease in the amplitude of the R waves and corresponding increase in the amplitude of S waves is seen in the right precordial leads. A persistent rightward axis can be indicative of congenital heart disease. 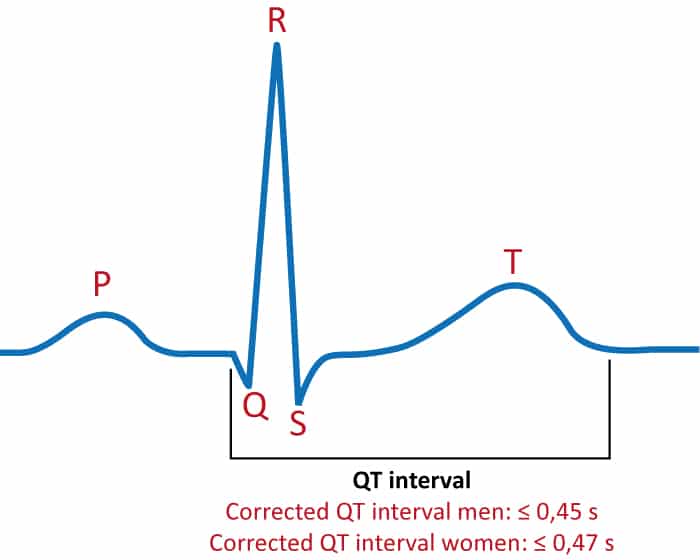
The normal adult ratio of right-to-left ventricle mass - and thus a normal axis - is expected to be seen by age 6 months. 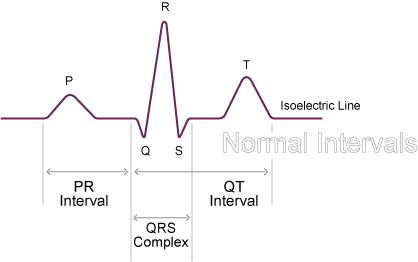
Most pronounced at 1-2 months of age, the axis slowly migrates from right to left as the left ventricular myocardium hypertrophies to account for the postnatal increase in systemic vascular resistance and a concomitant decrease in pulmonary vasculature pressures. 4Īt birth, all neonates have a rightward axis because of relative right ventricular hypertrophy. Up to 50% of infants can have sudden prolongation of the P-P interval with no symptomatic or long-term effects. This phenomenon is termed sinus arrhythmia. The resting heart rate does not coincide with adult range until at least age 5 years.Ĭhildren can also have wider variation in heart rate associated with the respiratory cycle and changes in P-P interval. Unlike adults, children not only tolerate a much higher heart rate but depend on an increase in heart rate alone to increase cardiac output. This review will focus on the key differences in rate, axis, and intervals. Detecting these differences can focus your differential, impact your treatment, and most importantly provide you with solid footing in making a relevant consultation to pediatric cardiology. The pediatric ECG has numerous subtle and not-so-subtle differences when compared to the average adult ECG. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
